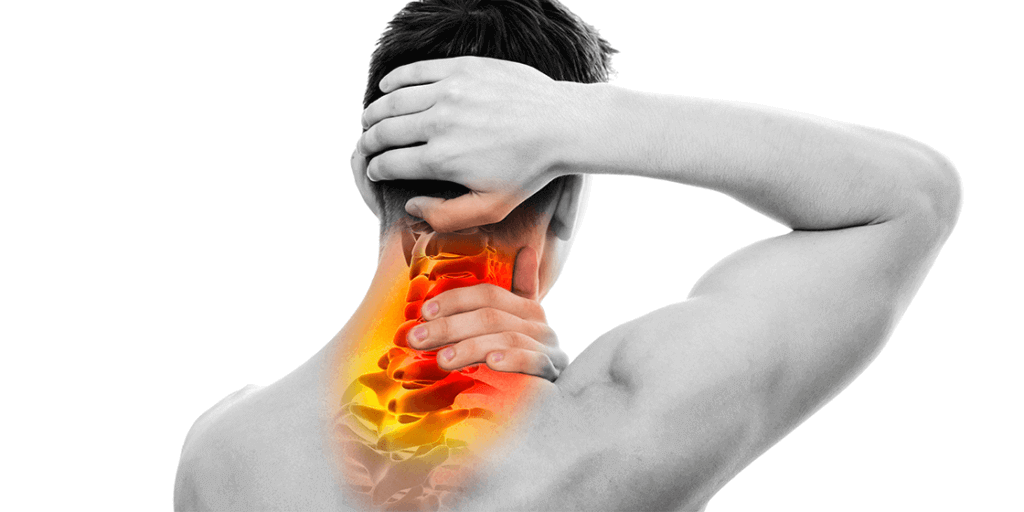
Why do I have a severe headache and neck pain at the base of my skull? Is this a tension headache? Is this a migraine? Do I have a brain tumor? These are all questions that undoubtedly roll through your mind when a headache kicks-in the back of your head and neck. Below we talk about the common types of headaches and how they are different. We explain what that pain behind your head and neck could mean. And we review forms of treatment for severe head and neck pain.
Types of headaches
Headaches can be a pain in the neck, both literally and figuratively. The cause of this pain can be due to a variety of reasons, ultimately resulting in a diagnosis of “headache.” There are many types of headaches which are differentiated by the cause of symptoms. We will review tension headaches, cervicogenic headaches and migraines. But what is causing the headache? Is it a disruption in your nervous system? Is it muscle tension in your neck from finishing up a deadline at work? While symptoms of different types of headaches can overlap, it can become challenging or confusing to diagnose. What is important is if you are currently receiving treatment for your headache and neck pain, you need to ask yourself, “is this treatment helping?” “Do I feel better?” Sometimes we take advice from a medical professional as FACT when in truth, we/they are practicing medicine. If a treatment is not actually helping to reduce your symptoms and it’s underlying causes then why not consider another option? Why not consider that your migraine may in fact be a recurring tension headache? Or maybe your neck and head pain is really a migraine in disguise. Below we dive further into the three most commonly seen reasons for headaches and neck pain: tension headaches, cervicogenic headaches and migraines.
Tension headaches
Tension headaches are the most common type of headache which are also referred to as “ordinary headaches, muscle- tension headaches and stress headaches.” Since there are many terms, for this “ordinary headache” the International Headache Society (it’s a real thing) suggests the term “tension-type headache” for clarity purposes. Individuals who are experiencing a tension-type headache tend to report generally diffuse, mild-moderate pain accompanied by a “tight band” or “vise” around their head. Compared to other headaches we will discuss, tension-type headaches are NOT accompanied by nausea, do not have a pulsating quality to the symptoms, and symptoms do not get worse with activity. Diagnosis of tension-type headache occurs via subjective reports of symptoms and review of medical history to rule-out other possible causes. The exact cause of tension-type headaches is unknown. Some believe changes in how the nerves of the head, neck, and shoulders sense pain are the root cause, while others suggest changes in how the brain interprets these pain signals, is the root cause. What we tend to see clinically, is someone presenting with an imbalance in muscle length and strength of muscles of the head and neck. This imbalance creates increased tension or an abnormal pull in the muscles where they attach to the spine and skull, leading to a headache. Stress, inadequate sleep, and poor hydration are also factors to consider when addressing tension-type headaches. If tension-type headaches are infrequent, they can be managed with OTC (over-the-counter) medications including aspirin, ibuprofen (Advil, Motrin) and acetaminophen (Tylenol). Ice compress, heating pad, acupuncture, massage.
Cervicogenic headaches
While symptoms may be similar, a cervicogenic headache is slightly different from a tension-type headache in that the underlying cause is related to a condition in the neck/ cervical spine. This means any joint, muscle, ligament, nerve, related to your cervical spine, could be the cause for the headache and neck pain. Patients often describe a feeling of dull pain in the back of the neck, which can radiate up into the back of the head, and even further on to the temple, forehead or behind the eye. Pain is typically one-sided, but can occur on both. Addressing a cervicogenic headache with OTC medications may be helpful temporarily but symptoms will most likely return, since the underlying cause was never addressed. Are you someone who deals with severe neck pain and headache at the base of your skull? Do you experience recurring headaches behind your eye? You may be dealing with a cervicogenic headache and in this case an evaluation by a Doctor of Physical Therapy would be indicated to further identify the root cause of your symptoms.
Migraines
Migraines are a little more complicated than the previous two because we still don’t really understand the mechanism for what is happening to create the symptoms of a migraine. Broadly speaking, migraines are characterized by a recurrent, throbbing headache, which typically affects one side of the head and is usually accompanied by nausea and disturbed vision. About ⅓ of migraine sufferers experience auras (visual disturbances including zigzagging lines, flashing lights), and have a pulsating quality to them. Symptoms seem to be sensitive to light and sound. While other headaches can occur in the face, head and neck, migraines tend to occur primarily in the head, and generally speaking, symptoms tend to be more severe than a tension-type headache. Many common triggers for migraines include stress, with onset typically occurring after the stressful event. Migraines have many overlapping qualities with a tension-type headache, and can also appear as a sinus infection with a runny nose and nasal congestion. Confusing much? Again, this is when you need to ask yourself if the treatment you are receiving for your headache and neck pain is helping. If it isn’t, then let’s consider another type of headache as the possible cause of your symptoms.
Treatment for headaches and neck pain
So what can you do to help yourself? Ultimately one of the best ways to hone in on which type of headache you may be suffering from, keep a journal. Write down hours slept, water consumed, diet, and when/where/what your symptoms were when they begin, how long they last. As mentioned above, tension-type headaches may be managed well with OTC medications. Those same medications may treat the symptoms of migraines and cervicogenic headaches but if symptoms persist, it may require further treatment or assessment by a physical therapist. Other conservative forms of managing symptoms include, cold compress, heat pack, foam roller to thoracic spine, massage, and other forms of stress-management.
Try out something new if what you have been doing isn’t working any longer. Contact us and we can help.
Lindsay Mercier, PT, DPT, OCS
Tags: physical therapy, health and wellness, headache, neck pain